Disease Management
A SUPPORT system for case managers
Disease management is a core business strategy that creates an opportunity to protect an employer’s investment in human capital. Many employer plan sponsors are realizing the benefits and effectiveness of staffing on-site disease management facilities/nurses. This supports the integrated care approach aligning wellness, Rx compliance, disease management and critical care. Med-Vision helps coordinate with case managers and onsite vendors for monitoring and measuring – thus, providing a complete support system in your efforts to reach out and help people.
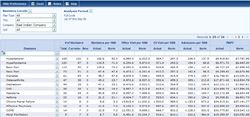 The current industry standard in disease management relies on telephonic member engagement. Typically, the process involves the identification of 10% of the member population considered “high risk” who are then contacted by nurses. A typical result will be 10-20% of this 10% identified population agreeing to ongoing telephonic nurse coaching (1 -2% of the member population). The current industry standard in disease management relies on telephonic member engagement. Typically, the process involves the identification of 10% of the member population considered “high risk” who are then contacted by nurses. A typical result will be 10-20% of this 10% identified population agreeing to ongoing telephonic nurse coaching (1 -2% of the member population).
(click on image to enlarge)
Identifying SOLUTIONS to improve conditions
Med-Vision believes the typical result mentioned above is not sufficient to lower cost or improve quality outcomes. In turn, Med-Vision provides the following solutions:
- Utilizing Med-View for member care-gap modeling methodology, members at high risk for future adverse medical events, and resulting high cost, are identified.
- Med-View is the base of a system of integrated health care interventions and communications that are actionable and client-specific.
- This technique also offers the opportunity to mitigate the progress and reduce the consequences of chronic health conditions.
Med-Vision clients are seeing decreased costs and improved clinical, financial, quality, and utilization metrics. Contact Med-Vision today for a health plan assessment and ensure a profitable and healthy future for you, your employees, and your organization.
|


